Birth control has long been a controversial topic, with debates raging over its accessibility, side effects and impact on society. One of the most concerning and debated issues is the birth control blood clot. Do birth control pills have the potential to cause a blood clot?
While many women rely on contraception to prevent pregnancy, there have been concerns raised about the safety of some forms in relation to blood clot formation, particularly with birth control pills. With conflicting information and fear-mongering circulating online, it can be overwhelming for women to navigate through this issue.
In this post, Dr. Michelle Chia, Medical Director of Ezra Clinic, shares insights from her personal experience and discusses the connection between birth control pills and potential blood clots. She also addresses common misconceptions and provides helpful insights for those considering or currently using hormonal birth control methods.
Understanding Blood Clots
Blood clots, or thrombosis, occur when blood coagulates and forms a semisolid mass. They can be beneficial in stopping bleeding/ blood flow but can also become dangerous blood clots when they form inappropriately.
Blood clots can be caused by various factors, including prolonged immobility, undergone major surgery, certain medications (such as combined oral contraceptives), and underlying health conditions. They can also be associated with genetic or hereditary factors. While combination hormonal methods increase the risk of blood clots, it is important to understand that this is still very rare. Birth control pills like the combination pill or other hormone-based birth control are still very safe to use.
It is important to consult with a doctor to see if you are suitable to start on birth control pills.
The two types of blood clots are:
Deep vein thrombosis (DVT)
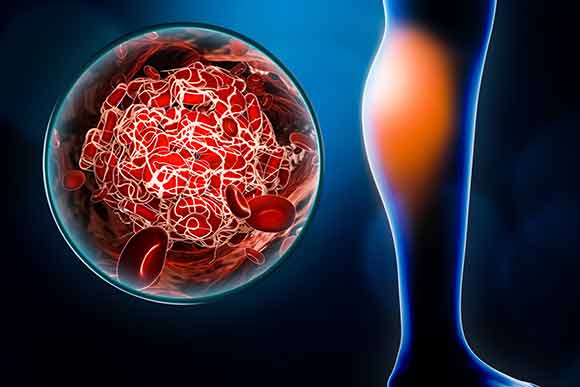
Deep vein thrombosis (DVT) is characterized by blood clot formation in the deep veins, typically in the legs and arms, mesenteric, and cerebral veins. This is due to slowed blood flow and clotting factors that cause the increased risk. DVT is considered an important disease, which can lead to serious complications if not diagnosed and treated promptly.
The development of venous thromboembolism can be influenced by many other factors apart from contraceptive pills. This includes prolonged immobility, any recent medical procedure, certain other health problems, hormone therapy and lifestyles like smoking and obesity. While individuals taking hormonal birth control pills may be at a slightly increased risk of developing DVT, it is important to understand that blood clots with birth control pills are uncommon and a rare occurrence if it is prescribed safely and appropriately.
Pulmonary embolism (PE)
A pulmonary embolism is a serious illness where a blood clot, usually from the legs’ deep veins, travels to the lungs and blocks the blood flow in the lung arteries. It leads to a decrease in oxygen levels in the blood and damage to the lung tissue.
PE can be life-threatening, especially if the clot is large or if there are multiple clots. The symptoms of PE include shortness of breath, chest pain, coughing up blood, rapid breathing, increased heart rate, and lightheadedness.
PE can be prevented by taking measures to prevent abnormal clotting, such as regular exercise, good chronic disease control and maintaining a healthy lifestyle like stopping smoking.
Blood Clot Common Misconception
The concern about contraception increasing the risk of blood clots, such as with birth control pills, patches, and rings, has led to unnecessary fear and hesitation due to certain misconceptions. While it is true that a combination of hormonal methods increases the risk of blood clots, the actual risk is generally low and varies on individual health factors. For instance, the risk of developing blood clots is significantly greater in pregnant women than those taking oral birth control pills.
The National Women’s Health Network emphasizes that blood clots are generally rare, even in otherwise healthy people, and that some personal characteristics and medical conditions increase the risk of blood clots. It includes obesity, genetic clotting disorders, blood problems, a broken hip, smoking, being over age 60, and prolonged inactivity. It’s important for individuals to be aware of factors that increase their blood clot risk, such as smoking or obesity, and to discuss their concerns with a healthcare provider when considering birth control options.
While it’s essential to be informed about the potential risks, it’s also important to consider the benefits of contraception and make decisions based on individual health factors, treatment guidelines and medical advice.
What actually causes Blood Clots?
Several studies suggest that the use of hormonal contraceptives like birth control pills is associated with a slightly elevated risk of blood clots compared to those who don’t use them, but the overall risk remains relatively very low. For example, combined hormonal contraceptives associated with the increased risk of blood clots are roughly 10 in 10,000 individuals on estrogen-containing birth control per year. The relative risk of thrombosis on combination birth control pills is three- to fivefold, whereas the absolute risk for a healthy individual on this therapy is only 0.05% per year.
Risk Factors for Blood Clots
While it is essential to discuss the various risk factors, it is also important to reiterate that the incidence of blood clots associated with birth control pills, a birth control patch, and birth control implants is generally low. Nevertheless, it is crucial to be aware of and understand how certain lifestyle choices and health conditions can increase the risk.
Smoking

Smoking has a well-documented impact on cardiovascular health and is known to significantly increase the risk of blood clots. Blood clots increase with smoking due to chemicals and toxins that cause increased clotting. Chemicals in cigarettes can damage blood vessels’ linings, leading to a higher propensity for clot formation.
Obesity
Carrying excess weight is a greater risk for venous thromboembolism than the combination pill. The increased pressure in the veins in your legs and pelvis can lead to blood clots. Obesity also leads to a state of increased inflammation in the body, contributing to reduced blood flow and clot risks.
Immobilization
Extended periods of immobility, such as long flights or bed rest after hip surgery, can impede the normal circulation of blood, particularly in the lower limbs, thereby increasing the risk of clot formation.
Family History
Genetic factors can be a significant factor in the risk of blood clots. A family history of clotting disorders may indicate a higher predisposition to developing blood clots.
How to Reduce the Risk of Blood Clots?

Stay Active: Regular physical activity and avoiding long periods of immobility can help prevent blood clots.
Maintain a Healthy Weight: Being obese or overweight increases the risk of blood clots. It is so important to maintain a healthy weight.
Avoid Smoking: Smoking increases the risk of blood clots, so quitting smoking is beneficial for reducing the risk.
Stay Hydrated: Dehydration increases the risk of developing a blood clot, so it’s important to drink plenty of water each day.
Know Your Family History: Understanding your family’s history of blood clots can help assess your own risk.
Choose Contraceptives Carefully: Consulting with an experienced doctor to evaluate your suitability for hormonal forms of contraception is important. High-risk patients will be advised to avoid certain methods of birth control.
Seek Medical Advice Before Surgery: Before any surgery, it’s important to talk to your doctor about the risk of developing blood clots and what preventive measures can be taken.
Conclusion
Birth control and blood clots have sparked much debate regarding their connection. Thrombosis can occur naturally or due to certain factors, including immobility, surgery, or medications like hormonal contraceptives. Birth control pills can increase the risk of deep vein thrombosis and pulmonary embolism, but it’s important to note that while the risk is heightened, it is still relatively low.
Misconceptions about the extent of this risk can cause undue fear; in reality, while contraceptives do increase the risk, pregnancy involves a significantly higher risk of blood clots. Factors such as obesity, genetic conditions, and smoking can further elevate the risk.
It’s vital for individuals to understand their personal health risks and consult with healthcare providers when choosing birth control methods. The overall incidence of blood clots with hormonal birth control is low but should be understood in the context of individual health and risk factors.








