What a PCOS Diagnosis Actually Means
PCOS is a syndrome, not a single disease
You can think of PCOS as a pattern, not a single fault with one clear test. The word syndrome means a group of signs and symptoms that tend to occur together. PCOS sits under reproductive endocrinology, which is the part of medicine that looks at how hormones affect periods, ovulation, and fertility. You can have PCOS even if one test looks normal. You can also have similar symptoms without PCOS, which is why doctors check the overall picture and rule out other causes.Why do symptoms vary between women
You might notice changes in your period, acne, hair growth, scalp hair thinning, weight changes, or difficulty conceiving. Another person might have only one or two of these. Symptoms vary because PCOS can involve different drivers, such as:- Ovulation patterns that are irregular
- Higher androgen levels (androgens are hormones such as testosterone)
- Differences in how your body responds to insulin (insulin is a hormone that helps control blood sugar)
Why diagnosis can change over time
You might meet the criteria at one point, then fall outside them later, or vice versa. Your cycle pattern can shift with age, stress, weight change, pregnancy, or stopping hormonal contraception. Ultrasound findings can also change, especially in younger women. A doctor often treats the diagnosis as a working conclusion based on current evidence, then updates it as your symptoms and results evolve. This approach refrains from over-labelling while still letting you act on what matters for your health.The Rotterdam Criteria Explained

What the Rotterdam Criteria are
doctors often use the Rotterdam Criteria to diagnose PCOS in adults. This framework helps your doctor avoid relying on one result, such as one blood test or one ultrasound image. Your doctor looks for a consistent pattern across your cycle history, symptoms, and investigations. You might see the anchor text PCOS diagnosis used in clinic education materials because it reflects this structured, criteria-based approach rather than a single “yes or no” test.The “two out of three” rule
The Rotterdam Criteria use a practical rule: you meet the diagnosis when you have two out of three features, after other conditions are ruled out. The three features are:- ovulatory dysfunction (your ovulation is irregular, often seen as irregular or absent periods)
- hyperandrogenism (higher androgen effects, seen in symptoms or blood results)
- polycystic ovarian morphology on ultrasound (an appearance that suggests more small follicles than expected)
When doctors use different diagnostic frameworks
doctors may adapt the diagnostic approach based on age, life stage, or hormonal use. Adolescents and people using hormonal contraception often need more cautious interpretation to avoid over- or under-diagnosis.What the criteria do not say
The Rotterdam Criteria do not, on their own, confirm the cause of your symptoms. The criteria do not tell you how severe your PCOS is. The criteria also do not guarantee fertility outcomes. The criteria do not mean you “must have cysts”. The ultrasound feature refers to ovarian appearance, not dangerous cysts. Your doctor still needs to rule out other conditions that can look similar before confirming the diagnosis.Doctor’s Insight:
Many women expect one test to confirm PCOS, but in practice, diagnosis is rarely that simple. We often see patients who have one strong feature but fall short on another, especially at different life stages.
Often times, we also see varied features on hormone tests or ultrasound findings. Some women may only show signs on the hormone test, while some only on ultrasound, while some have both. So it is crucial to do proper examination and evaluation to get the full picture for a proper diagnosis.
Criterion 1: Ovulatory Dysfunction
What “irregular ovulation” means in practice
Ovulatory dysfunction means you do not ovulate regularly. Ovulation is when your ovary releases an egg. You usually see ovulation problems through your cycle pattern, because irregular ovulation often leads to irregular periods. You can still bleed without ovulating, so your doctor looks beyond whether you “get a period” and focuses on timing, consistency, and change over time.Cycle patterns that raise suspicion
- Oligomenorrhoea (infrequent periods)
- Amenorrhoea (absent periods)
- Your doctor also considers patterns such as frequent missed periods and cycles that vary widely month to month. Bleeding that becomes unusually long or delayed may fit heavy, prolonged, or delayed menstruation.
- Your doctor also pays attention to bleeding that occurs outside expected periods, as this can point to a different issue that needs checking. This pattern is covered in bleeding between periods.
How doctors assess ovulation
- Menstrual history
- Ovulation tracking basics
- Progesterone timing (what it can and cannot show)
Common pitfalls
Stress, travel, weight change, and stopping hormonal contraception can all temporarily disrupt ovulation. doctors usually consider these factors before confirming PCOS to avoid labelling short-term changes as a chronic condition.Criterion 2: Hyperandrogenism
Clinical hyperandrogenism (symptoms you can see)
Clinical hyperandrogenism means your body shows visible signs of higher androgen activity. Androgens are hormones such as testosterone. Women need small amounts, but higher activity can affect skin and hair. Your doctor may ask about:- hirsutism (coarser, darker hair growth on areas such as the chin, upper lip, chest, lower abdomen, or inner thighs)
- acne, especially persistent or jawline acne, often described as hormonal acne
- scalp hair thinning, often described as female pattern hair loss
Biochemical hyperandrogenism (blood results)
Biochemical hyperandrogenism means blood tests show higher androgen levels. Common tests include:- total testosterone
- free testosterone (the portion not bound to proteins)
- DHEAS (dehydroepiandrosterone sulfate), which can reflect adrenal androgen production
- androstenedione
Why symptoms and blood tests do not always match
You can have symptoms with “normal” blood levels. You can also have mildly raised levels without obvious symptoms. Several factors can explain this:- Your hair follicles and skin can be more sensitive to normal androgen levels
- Hormone levels can fluctuate
- Some tests measure hormones more accurately than others
When doctors consider other causes of high androgens
Your doctor checks for red flags that suggest a different cause, especially if symptoms start suddenly or progress quickly. Your doctor may consider other conditions that can raise androgens, which is one reason exclusion testing is part of a safe PCOS workup.Criterion 3: Polycystic Ovarian Morphology on Ultrasound
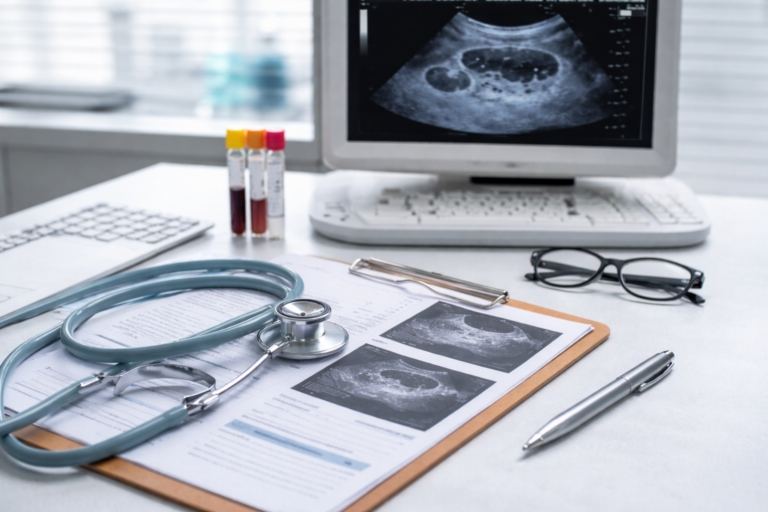
 What an ultrasound can and cannot diagnose
An ultrasound shows how your ovaries look at a point in time. It can describe ovarian size and the number of small follicles present, but it cannot diagnose PCOS on its own. A scan does not explain why these features are present, and it does not confirm how your hormones or ovulation are functioning.
Your doctor uses ultrasound findings alongside your symptoms, cycle history, and blood tests as part of an overall assessment.
Polycystic ovarian morphology vs PCOS
Polycystic ovarian morphology refers to an ovarian appearance that meets ultrasound criteria used in PCOS assessment. This appearance can occur in people with PCOS, but it can also be seen in people without the condition.
You can meet diagnostic criteria for PCOS without this ultrasound feature. You can also have this ovarian appearance without having PCOS. This is why doctors avoid diagnosing PCOS based on a scan alone.
Why “cysts” is a misleading word
The word cysts often causes unnecessary concern. The small round structures seen on ultrasound are follicles, not harmful cysts. Follicles are normal structures that contain immature eggs.
In PCOS, more follicles may be visible because ovulation does not occur regularly, not because something abnormal is growing in the ovary.
Factors that affect how ultrasound findings are interpreted
Ultrasound interpretation depends on scan type, image quality, age, and hormonal use. A transvaginal scan usually gives clearer ovarian images than a transabdominal scan, but a transabdominal scan may be used when a transvaginal scan is not suitable. These factors affect how clearly follicles and ovarian volume can be assessed, which is why scans are interpreted in context rather than used alone to diagnose PCOS.
When ovaries look “normal” in PCOS
You can still meet diagnostic criteria for PCOS even if your ovaries appear normal on ultrasound. In these cases, ovulatory dysfunction and hyperandrogenism carry more diagnostic weight.
Your doctor focuses on the full clinical picture rather than relying on ovarian appearance alone.
What an ultrasound can and cannot diagnose
An ultrasound shows how your ovaries look at a point in time. It can describe ovarian size and the number of small follicles present, but it cannot diagnose PCOS on its own. A scan does not explain why these features are present, and it does not confirm how your hormones or ovulation are functioning.
Your doctor uses ultrasound findings alongside your symptoms, cycle history, and blood tests as part of an overall assessment.
Polycystic ovarian morphology vs PCOS
Polycystic ovarian morphology refers to an ovarian appearance that meets ultrasound criteria used in PCOS assessment. This appearance can occur in people with PCOS, but it can also be seen in people without the condition.
You can meet diagnostic criteria for PCOS without this ultrasound feature. You can also have this ovarian appearance without having PCOS. This is why doctors avoid diagnosing PCOS based on a scan alone.
Why “cysts” is a misleading word
The word cysts often causes unnecessary concern. The small round structures seen on ultrasound are follicles, not harmful cysts. Follicles are normal structures that contain immature eggs.
In PCOS, more follicles may be visible because ovulation does not occur regularly, not because something abnormal is growing in the ovary.
Factors that affect how ultrasound findings are interpreted
Ultrasound interpretation depends on scan type, image quality, age, and hormonal use. A transvaginal scan usually gives clearer ovarian images than a transabdominal scan, but a transabdominal scan may be used when a transvaginal scan is not suitable. These factors affect how clearly follicles and ovarian volume can be assessed, which is why scans are interpreted in context rather than used alone to diagnose PCOS.
When ovaries look “normal” in PCOS
You can still meet diagnostic criteria for PCOS even if your ovaries appear normal on ultrasound. In these cases, ovulatory dysfunction and hyperandrogenism carry more diagnostic weight.
Your doctor focuses on the full clinical picture rather than relying on ovarian appearance alone.
Blood Tests Used in PCOS Workups
Tests that support the overall picture
Blood tests do not “prove” PCOS on their own. Blood tests support what your symptoms and cycle pattern already suggest. Your doctor usually chooses tests that answer specific questions, not a long list “just in case”.- Androgens
- Metabolic screening (glucose, lipids)
Tests used to rule out other conditions
A safe PCOS workup also checks for conditions that can mimic PCOS. This exclusion step matters because treatment choices change when the underlying cause is different.- Thyroid function (TSH: thyroid-stimulating hormone)
- Prolactin
- 17-hydroxyprogesterone
- Other tests when indicated
The LH–FSH ratio: why it is not a diagnosis
You may come across the LH–FSH ratio online as a “PCOS test”. While some people with PCOS have a higher luteinising hormone (LH) relative to follicle-stimulating hormone (FSH), this pattern is inconsistent and can also appear in people without PCOS. LH is released in pulses, so a single blood test may not reflect typical levels. doctors may measure LH and FSH to support the overall assessment or exclude other conditions, but the ratio does not diagnose PCOS.AMH (anti-Müllerian hormone): when it helps, when it misleads
AMH reflects the number of small follicles in the ovaries and is often higher in people with PCOS. It can support the overall clinical picture, particularly when ultrasound findings are unclear. However, AMH varies with age and testing method and cannot diagnose PCOS on its own. Current international guidelines do not recommend using AMH as a standalone diagnostic test.Conditions That Mimic PCOS
Several conditions can cause symptoms similar to PCOS. doctors usually check for these early because the correct diagnosis affects both safety and treatment decisions. Most guidelines recommend ruling out a small group of key conditions before confirming PCOS.Thyroid disorders
Thyroid imbalance can disrupt ovulation and menstrual cycles, which is why thyroid-stimulating hormone (TSH) is routinely checked in people with irregular periods.Hyperprolactinaemia
Raised prolactin levels can interfere with ovulation and cause absent or irregular periods, so prolactin is commonly tested before confirming PCOS.Non-classic congenital adrenal hyperplasia
This inherited adrenal condition can raise androgen levels and cause acne, excess hair growth, and cycle irregularity, and is typically screened for using 17-hydroxyprogesterone.Hypothalamic amenorrhoea
This condition involves reduced hormone signalling from the brain, often related to stress, energy deficit, weight loss, or heavy exercise, and usually presents without the androgen pattern seen in PCOS.Cushing syndrome and rare androgen-secreting tumours (when suspected)
These are uncommon but considered when symptoms develop suddenly, worsen rapidly, or suggest cortisol excess rather than a typical PCOS pattern.Why ruling out matters for safety and treatment choices
Ruling out these conditions helps avoid misdiagnosis and ensures that treatment targets the true cause of symptoms, which is why PCOS diagnosis involves both meeting criteria and excluding look-alike conditions.PCOS Phenotypes and Why Your Presentation Matters
What “phenotype” means
A phenotype describes the pattern of diagnostic features you have within PCOS. doctors use phenotypes to group presentations based on the Rotterdam Criteria, because PCOS does not look the same in everyone. This helps guide assessment and follow-up, rather than defining a fixed outcome.The four Rotterdam phenotypes (A–D) in plain language
PCOS phenotypes are described using three features: ovulatory dysfunction, hyperandrogenism, and polycystic ovarian morphology on ultrasound. Phenotype A (all three features) Irregular or absent ovulation, signs of higher androgens, and polycystic ovarian morphology on ultrasound. Phenotype B (ovulation + androgens) Irregular or absent ovulation and signs of higher androgens, without polycystic ovarian morphology on ultrasound. Phenotype C (androgens + ultrasound) Signs of higher androgens and polycystic ovarian morphology, with more regular ovulation. Phenotype D (ovulation + ultrasound) Irregular or absent ovulation and polycystic ovarian morphology, without clear signs of higher androgens.How phenotype affects symptoms, risks, and next steps
Your phenotype can influence which symptoms are most noticeable and what your doctor prioritises during assessment. Some patterns are more associated with skin or hair concerns, while others relate more to menstrual regularity or fertility timing. doctors use phenotype as a guide, not a label, and focus on managing the issues that matter most to you.Common Misconceptions That Delay Diagnosis
You might read confident claims online that sound simple, but PCOS rarely works that way. You often save time and unnecessary anxiety when PCOS is understood as a criteria-based pattern, rather than a diagnosis made from a single scan or one blood test. International guidelines highlight that inconsistent understanding of diagnostic criteria is a common reason for delayed or unclear diagnosis.“You must have cysts to have PCOS”
You do not need “cysts” to meet PCOS criteria. Ultrasound looks for polycystic ovarian morphology, which describes many small follicles, not harmful cysts. You can meet diagnostic criteria through ovulatory dysfunction and androgen features even when ultrasound findings are not present.“Regular periods mean you cannot have PCOS”
You can have PCOS with relatively regular bleeding. Ovulation can still be irregular even when periods appear predictable. You can also meet diagnostic criteria through hyperandrogenism and ultrasound findings. Your doctor assesses the full pattern rather than using regular periods as a rule-out.“An ultrasound alone confirms PCOS”
An ultrasound cannot confirm PCOS on its own. Ultrasound supports the assessment, but doctors also consider cycle patterns, androgen features, and exclusion testing for conditions that can look similar.“AMH confirms PCOS”
AMH (anti-Müllerian hormone) can be higher in many people with PCOS because it reflects the number of small follicles in the ovaries. AMH does not diagnose PCOS by itself, as levels vary by age and testing method. Current guidance does not support AMH as a standalone diagnostic test.“PCOS only affects people who are overweight”
You can have PCOS at any body size. Weight can influence insulin resistance and symptom severity for some people, but it does not define the condition.“PCOS always causes infertility”
PCOS can make ovulation less predictable, which may affect how long it takes to conceive. PCOS does not mean you cannot get pregnant. Many people conceive with appropriate timing support or fertility care, which is discussed in more detail in PCOS and fertility.Diagnosis in Teenagers, Pill Users, and Later Adulthood
PCOS diagnosis can look different depending on age and hormonal context. At certain life stages, test results can overlap with normal physiology or be temporarily altered by contraception. Your doctor adjusts how strongly they rely on specific findings to avoid both over-diagnosis and missed diagnosis.Diagnosing PCOS in teenagers (why it is more complex)
During adolescence, irregular cycles, acne, and ovaries with many follicles can be part of normal puberty. This makes diagnosis less clear-cut. Current guidelines use stricter criteria for teenagers. Your doctor usually looks for persistent cycle irregularity several years after menarche plus clear signs of hyperandrogenism. If only one feature is present, monitoring over time is often preferred.Diagnosing PCOS while on hormonal contraception
Hormonal contraception can change bleeding patterns and can affect blood markers used to assess androgens. This can make results harder to interpret for PCOS diagnosis. Your doctor often relies more on your symptom history and menstrual pattern before contraception and may time testing carefully if stopping contraception is appropriate and aligned with your goals. Hormonal contraception can also be used to manage PCOS symptoms after diagnosis, which is covered in birth control for PCOS.Diagnosing PCOS after 35 and in perimenopause
PCOS can persist into later reproductive years, but cycles and ovarian appearance often change with age. Around perimenopause, ultrasound findings may no longer look typical. Your doctor places more weight on your long-term history of irregular ovulation and hyperandrogenism, rather than expecting current tests to meet classic diagnostic patterns.What to Expect at a PCOS Diagnostic Appointment
History and symptom review
Your appointment usually starts with a detailed conversation. Your doctor asks about your menstrual cycles, when changes began, and how regular or irregular they have been over time. You may also be asked about acne, hair growth, scalp hair thinning, weight changes, and any fertility concerns. Your past medical history is important. This includes previous blood tests, scans, pregnancies, use of hormonal contraception, and family history of hormonal or metabolic conditions. These details help your doctor decide which diagnostic criteria apply to you and which tests are actually needed.Physical assessment and investigation planning
A physical assessment may be part of the visit, depending on your symptoms and comfort. This can include checking blood pressure, weight, and body mass index, as well as looking for visible signs of higher androgen activity such as acne or hair pattern changes. Your doctor then plans investigations carefully rather than ordering everything at once. Blood tests may need to be timed to your cycle or medication use to avoid misleading results. Ultrasound type and timing are chosen based on your age and situation. You are told what preparation is needed, such as fasting for metabolic tests or scheduling follow-up scans.Follow-up and interpretation (how results are put together)
Results are not reviewed in isolation. Your doctor brings together your history, symptoms, blood tests, and scan findings to assess whether diagnostic criteria are met and whether other conditions have been ruled out. This follow-up is where PCOS is confirmed, considered unlikely, or monitored over time. You should leave with a clear explanation of what your results mean and what the next steps are, even if a final diagnosis is not made immediately.When Your Results Are Borderline or Unclear
Why doctors may monitor instead of label immediately
Sometimes your results sit near the diagnostic thresholds or only one criterion is present. In these situations, your doctor may avoid confirming a diagnosis straight away. This is not dismissal. It is a cautious approach that reduces the risk of over-diagnosis, especially when hormone levels, cycle patterns, or ultrasound findings may still be settling. Monitoring allows your doctor to see whether patterns persist over time. This approach is common in younger patients, after stopping hormonal contraception, or when symptoms are mild.When repeat testing helps
Repeat testing can be useful when timing or temporary factors may have influenced results. Hormone levels can vary between cycles, and ultrasound findings can change with age and hormonal state. Repeating tests after a defined interval can clarify whether findings are consistent or transient. Your doctor usually explains why repeat testing is recommended and what change they are looking for, so you know what the follow-up is meant to answer.Red flags that need faster review
Some features prompt earlier review or additional testing. These include rapidly worsening androgen-related symptoms, severe or sudden cycle changes, or symptoms that do not fit a typical PCOS pattern. If red flags are present, your doctor focuses on excluding other conditions quickly rather than waiting. This safety-first approach ensures that important diagnoses are not missed while still keeping PCOS in consideration where appropriate.Doctor’s Insights:
Different women may present with varying symptoms of PCOS and borderline results are common. It is therefore important to look at clinical symptoms and correlate them with the correct investigations as a whole for accurate diagnosis.
Monitoring is not about delaying care. It allows us to see whether changes persist and to rule out other causes that may need different treatment.
Next Steps After Diagnosis
What diagnosis does and does not change
A PCOS diagnosis gives you a clearer explanation for a pattern of symptoms. A PCOS diagnosis does not define your future health or fertility on its own. Your doctor uses the diagnosis to prioritise the right checks and the right next steps, based on what affects you most. You can also use the diagnosis to focus on prevention. Clinical guidance emphasises ongoing assessment of metabolic risk factors such as blood sugar and cholesterol, even when your main symptoms are menstrual or skin-related. If you want a practical overview of local care pathways, PCOS treatment in Singapore outlines common management options and what follow-up may involve.First-line management options by main concern
- Cycle regulation
- Acne and hair symptoms
- Fertility planning
- Metabolic health
How to track progress over time
You will usually make faster progress when you track what matters to your goals. You can track cycle timing, acne flare patterns, hair changes, weight trends, and any fertility milestones. You can also track key blood markers your doctor recommends, such as glucose and lipids, because PCOS care often involves ongoing risk monitoring rather than a one-off diagnosis.Conclusion
PCOS diagnosis works best when your doctor uses a combined, safety-first approach. You see clearer answers when your doctor reviews your cycle pattern, checks for androgen-related features, and uses ultrasound and blood tests to support the overall picture. You also benefit when your doctor rules out other conditions that can mimic PCOS before confirming the diagnosis. You can now interpret tests more realistically. You know that an ultrasound can describe ovarian appearance, but it cannot confirm PCOS on its own. You know that blood tests can support the assessment, but they rarely provide a single definitive result. You can also separate common myths from clinical criteria. You do not need “cysts” to have PCOS, and regular bleeding does not always rule it out. You can move forward with a clearer plan, whether that means monitoring, repeat testing, or focused management based on your main concern.Medical References
- Teede HJ, Misso ML, Costello MF, et al. International evidence-based guideline for the assessment and management of polycystic ovary syndrome (2023 update). Human Reproduction, 2023. https://academic.oup.com/humrep/article/38/9/1627/7241373 (Primary authority for diagnosis, adolescents, AMH, phenotypes, metabolic screening, and misconceptions)
- Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group. Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome. Human Reproduction, 2004. https://academic.oup.com/humrep/article/19/1/41/2356307 (Foundational source for the Rotterdam Criteria and the “two out of three” rule)
- Dewailly D, Lujan ME, Carmina E, et al. Definition and significance of polycystic ovarian morphology. Human Reproduction Update, 2014. https://academic.oup.com/humupd/article/20/3/334/620215 (Supports ultrasound interpretation and why “cysts” is misleading)
- Azziz R, Carmina E, Chen Z, et al. Polycystic ovary syndrome. Nature Reviews Disease Primers, 2016. https://www.nature.com/articles/nrdp201657 (High-level overview of PCOS as a syndrome, symptom variability, and pathophysiology)
- Lizneva D, Suturina L, Walker W, et al. Criteria, prevalence, and phenotypes of polycystic ovary syndrome. Fertility and Sterility, 2016. https://www.sciencedirect.com/science/article/pii/S0015028216000621 (Supports phenotype classification and why presentation differs)
- Legro RS, Arslanian SA, Ehrmann DA, et al. Diagnosis and treatment of polycystic ovary syndrome: an Endocrine Society clinical practice guideline. Journal of Clinical Endocrinology & Metabolism, 2013. https://academic.oup.com/jcem/article/98/12/4565/2833703 (Supports blood test selection, exclusion testing, and diagnostic cautions)
- American Academy of Family Physicians (AAFP). Polycystic Ovary Syndrome: Common Questions and Answers. American Family Physician, 2023. https://www.aafp.org/pubs/afp/issues/2023/0300/polycystic-ovary-syndrome.html (Clear support for exclusion of thyroid disease, hyperprolactinaemia, CAH, and common misconceptions)