Trying to get pregnant can feel like guesswork when your periods are irregular. You might track, wait, and still wonder if you even ovulated. That uncertainty is exhausting, especially when you want clear answers and a sensible plan.
Polycystic Ovary Syndrome (PCOS) is a common hormonal condition that often affects ovulation, which is the monthly release of an egg. Fertility with PCOS usually depends less on the label itself and more on how regularly you ovulate and how accurately you time sex around your fertile window.
This guide explains what is happening with ovulation, how to approach trying naturally in a realistic way, and how to improve your chances by supporting ovulation. It also shows you when it is time to seek an assessment, so you stop losing months to uncertainty.
PCOS and fertility: what changes and what does not
PCOS can delay conception because it often makes ovulation irregular. Ovulation is the release of an egg. Pregnancy usually depends on ovulation happening often enough and at a time you can identify. Many women with PCOS still get pregnant. Some conceive naturally. Others need support to restore more predictable ovulation. According to the National Institutes of Health’s MedlinePlus, PCOS is a hormonal condition that can affect ovulation and fertility, which helps explain why timing can become unpredictable. If you want a better understanding of what PCOS is and how it affects the body, you can read the full guide before you go further.
“Polycystic ovaries” can sound alarming, but it does not usually mean you have dangerous cysts. It often means your ovaries contain many small follicles. Follicles are fluid-filled sacs that hold immature eggs. In PCOS, these follicles can remain “stuck” in early growth stages because the hormonal signals that drive ovulation become disrupted. That pattern can be seen on ultrasound and is called polycystic ovarian morphology.
You might also hear about ovarian reserve and assume it equals fertility. Ovarian reserve describes your egg supply, not whether you regularly release an egg. Many women with PCOS have a good egg supply, but they ovulate less often. That is why treatment and lifestyle changes often focus on improving ovulation consistency and timing instead of “increasing egg count”.
Key takeaways you can remember quickly
- PCOS can delay pregnancy because ovulation can be irregular, not because pregnancy is impossible.
- Polycystic ovaries usually mean many small follicles, not harmful cysts.
- Ovarian reserve reflects egg supply, but ovulation determines timing and opportunity.
- Irregular periods often indicate fewer chances to conceive each year.
- A clear plan focuses on improving ovulation regularity and identifying your fertile window
Ovulation basics: how pregnancy starts each month
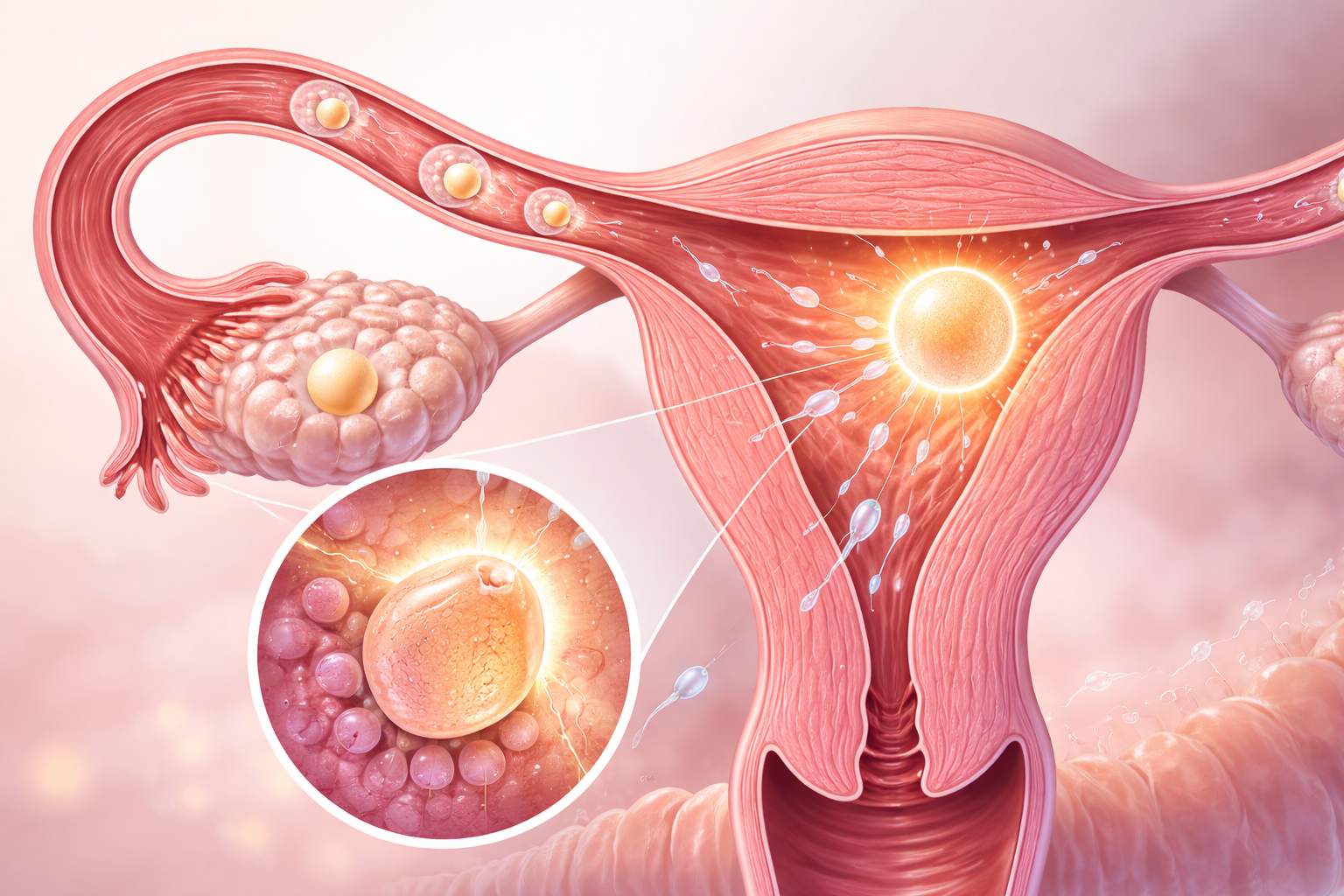
Ovulation is the key event that makes pregnancy possible. It happens when one egg matures and is released from the ovary. Pregnancy is most likely when sex is timed around this release.
You can think of ovulation in three simple steps. First, an egg matures inside a follicle. Second, the egg is released. Third, your body enters the luteal phase, when progesterone rises to support the uterine lining before your next period.
Regular cycles make timing easier because ovulation tends to follow a more predictable pattern. Irregular cycles make fertile days harder to identify, even when you do ovulate. Your fertile window is the set of days when pregnancy is most likely. It usually includes the day you ovulate and the five days before it. The National Health Service (NHS) explains that ovulation usually occurs before the next period and that pregnancy is most likely around the time of ovulation.
Signs you might be ovulating
- You notice clear, stretchy cervical mucus.
- You feel one-sided lower abdominal pain mid-cycle.
- You see a consistent cycle pattern across months.
Why PCOS disrupts ovulation
PCOS can disrupt ovulation because the hormonal signals that regulate your cycle become less coordinated. Your brain and ovaries communicate through hormones. Two key hormones are luteinising hormone (LH) and follicle-stimulating hormone (FSH). FSH supports early follicle growth. LH helps trigger ovulation when the egg is ready. In PCOS, LH levels are often relatively higher, and this imbalance can interfere with normal follicle development and ovulation. The Endocrine Society explains that disrupted LH and FSH signalling is a central feature of PCOS and contributes to irregular or absent ovulation.
PCOS can also involve higher androgen levels. Androgens are hormones that include testosterone. Women need small amounts of androgens, but higher levels can interfere with follicle maturation. Follicles may begin to grow but stall before reaching the stage needed for ovulation. These same androgen shifts often explain outward symptoms, such as skin changes, which are covered in more detail in this guide on PCOS and hormonal acne. This overlap reflects a shared hormonal mechanism rather than separate conditions.
Insulin resistance can add another layer. Insulin resistance means your body needs more insulin to keep blood sugar steady. Higher insulin levels can stimulate the ovaries to produce more androgens, further disrupting ovulation. The National Institutes of Health notes that insulin resistance is common in PCOS and plays a role in hormonal imbalance and ovulatory dysfunction. Not every woman with PCOS has insulin resistance, but it is common enough that it matters for fertility planning.
Anovulation and oligo-ovulation
Anovulation means ovulation does not happen. No egg is released, so pregnancy cannot occur in that cycle. Oligo-ovulation means that ovulation occurs but is infrequent or unpredictable. Both patterns can increase time to pregnancy because you have fewer true chances to conceive across a year. You might have bleeding, but you might not have released an egg.
Irregular periods and the “hidden” fertile window
Periods do not always confirm ovulation. Some bleeding can happen even when you do not ovulate, especially when hormone levels fluctuate. That can create false reassurance and make timing attempts harder. If you want a clearer explanation of how irregular periods behave and why they occur, it can help put this pattern into context.
Long cycles often indicate fewer ovulatory chances per year. A 28-day cycle gives you around 12 chances a year. A 45-day cycle gives you fewer cycles, and some of those cycles might not include ovulation at all. That is why many PCOS fertility plans focus on making ovulation more regular and easier to identify, instead of only “trying more often” without a clear window.
Can you get pregnant naturally with PCOS
Yes, a natural pregnancy is possible for many women with PCOS. It is more realistic when ovulation happens regularly, even if cycles are longer than average. If you ovulate, you have a chance to conceive. The challenge is often identifying when ovulation occurs and whether it occurs often enough throughout the year.
Time to pregnancy can be longer with PCOS because ovulation may be irregular or infrequent. You might ovulate some months and not others. You might also ovulate later in the cycle, which narrows your fertile window. This does not mean something is “wrong” with you. It means your body needs more accurate timing and, in some cases, support to improve consistency.
Consistent tracking matters more than guesswork. Having sex frequently without knowing whether ovulation is happening can feel proactive, but it can also lead to months of uncertainty. Tracking helps you understand your own pattern and decide when trying naturally is still reasonable and when waiting longer is unlikely to help.
Lean PCOS vs weight-associated PCOS
Lean PCOS describes PCOS in women who are not overweight. Weight-associated PCOS describes PCOS that occurs alongside higher body weight. Fertility patterns can differ, but weight alone does not determine whether you ovulate or conceive. Your cycle pattern, insulin sensitivity (how well your body responds to insulin), and signs of androgen excess often give a clearer picture than the number on the scale.
- You ovulate regularly, so timing is usually the main issue.
- You ovulate irregularly, so tracking and cycle support matter more.
- You do not ovulate, so assessment and targeted support often save time.
- You have metabolic issues, so improving insulin sensitivity can support more consistent ovulation.
PCOS phenotypes and fertility patterns
PCOS does not look the same in everyone. Fertility patterns usually fall into a few broad groups.
- If you ovulate regularly, your main challenge is often timing, not egg release.
- If you ovulate irregularly, tracking and cycle support become more important.
- If you do not ovulate, waiting without assessment usually delays pregnancy.
- If metabolic issues are present, addressing them can improve ovulation consistency.
Understanding which pattern fits you helps you choose the right next step rather than applying advice that does not match your body.
How to track ovulation with PCOS without getting misled
Tracking ovulation should help you make decisions. It should not turn into a long-term project that keeps you stuck. With PCOS, ovulation can be unpredictable, so tracking works best when you look for broad patterns rather than perfect predictions.
Irregular cycles often need more than one signal. One method may suggest a possible fertile window. Another can help confirm what actually happened. If tracking remains unclear after several cycles, that uncertainty is useful information. It often signals that it is time to assess ovulation more directly instead of continuing to guess.
Ovulation predictor kits: when they help and when they do not
Ovulation predictor kits detect a rise in luteinising hormone (LH), which usually happens before ovulation. In PCOS, LH levels can be higher at baseline or surge more than once, which can lead to false positives.
A positive result may point to a fertile window, but it does not confirm ovulation. Repeated positives across many days usually indicate unclear signalling, and should guide next steps rather than extend uncertainty.
Basal body temperature and cycle charting
Basal body temperature rises after ovulation due to hormonal changes. A sustained rise can confirm that ovulation likely occurred, but it cannot reliably predict ovulation in advance.
This method is most useful when you review patterns across several cycles. If temperature shifts remain inconsistent, tracking alone may not provide the clarity you need.
When to consider ultrasound or blood tests for ovulation confirmation
Clinical confirmation helps when cycles are long, tracking signals conflict, or months pass without confidence that ovulation is happening. Ultrasound can show whether follicles are developing towards ovulation. Blood tests can check progesterone after a suspected ovulation window to confirm whether ovulation occurred.
This approach saves time by replacing guesswork with confirmation. For many women with PCOS, that clarity makes it easier to decide whether to keep trying naturally or move forward with targeted support.
What you can do now to improve ovulation chances
You can take steps now that support more regular ovulation, even before you decide on medical assessment. You should aim for steady progress, not perfection. Extreme dieting or over-exercising can raise stress hormones and make cycles less predictable. Your goal is consistency that your body can maintain.
Small, repeatable changes often work better than major changes you cannot sustain. These habits help stabilise energy levels and support insulin sensitivity. Insulin sensitivity describes how well your body responds to insulin, which helps regulate blood sugar. Better insulin sensitivity can support more stable hormone signalling in many women with PCOS. If ovulation remains unclear after these changes, lifestyle support alone may not be enough.
Nutrition principles that support insulin sensitivity
You do not need a restrictive plan. You need an approach you can follow most days.
- You build meals around protein, fibre, and healthy fats to reduce sharp blood sugar rises.
- You choose minimally processed carbohydrates more often, such as brown rice, oats, and wholegrain bread.
- You include vegetables at lunch and dinner, including local options such as kai lan, bok choy, and cabbage.
- You reduce sweet drinks and choose water, unsweetened tea, or kopi and teh with less sugar.
- You keep rice or noodle portions consistent, especially when eating at hawker centres.
Physical activity that supports hormone balance
You do not need intense workouts to see benefits. You need regular movement to improve insulin sensitivity and support mood. Walking is a strong baseline, especially after meals. Resistance training also helps, because muscle improves how your body uses glucose.
You should prioritise consistency over intensity. Three to five manageable sessions each week usually support hormone balance better than infrequent high-intensity exercise followed by fatigue.
Sleep and stress: why they matter more than most people think
Stress and poor sleep can affect ovulation by influencing cortisol levels. Cortisol is a hormone released under stress. Persistently high cortisol can interfere with other hormone signals and can worsen insulin resistance for some women.
You can support this area with simple steps:
- You keep a consistent wake time most days.
- You start a short wind-down routine before sleep.
- You reduce late caffeine, especially in the afternoon and evening.
When trying longer does not help: clear signs it is time to seek support
Trying for longer only helps if ovulation is happening often enough to give you real chances to conceive. If ovulation is rare, unpredictable, or absent, time can pass without improving your odds. Support does not mean you have failed. Support means you stop relying on guesswork and start working with clear information.
You should also consider age and cycle pattern together. Age affects egg quality over time. Cycle pattern affects how many chances you get each year. A sensible threshold respects both.
Time-based thresholds
Many guidelines use a simple rule. You seek assessment after 12 months of trying if you are under 35 and having regular sex without contraception. You seek assessment after 6 months if you are 35 or older. The reason is practical. Fertility can decline with age, so waiting longer can reduce options.
Irregular cycles can shorten the wait time at any age. If you have long gaps between periods, you may not be ovulating regularly. Waiting 12 months when you only ovulate a few times a year can mean you have had very few real chances to conceive. An earlier assessment can save time and reduce stress.
Cycle-based thresholds
You should consider seeking support sooner if any of these apply.
- You have very long cycles, such as more than 35 days, especially if they vary widely.
- You frequently miss periods or go months without bleeding.
- You have no clear signs of ovulation across several cycles, even with tracking.
These patterns often signal infrequent ovulation or anovulation. An assessment can confirm what is happening and clarify your options.
Health-based thresholds
You should also seek support earlier if health factors may be affecting ovulation or pregnancy risk.
- You have known insulin resistance or markers of prediabetes, such as raised fasting glucose or raised HbA1c. HbA1c is a blood test that reflects average blood sugar over about three months.
- You have severe PCOS symptoms that affect daily life, such as significant fatigue, distressing hair or skin changes, or mood symptoms.
- You have experienced a previous pregnancy loss. You deserve a careful review and a plan that supports both conception and early pregnancy health.
Doctor’s Insights: Many women with PCOS delay seeking an assessment for their fertility because they are still having periods. From a clinical perspective, the key question is whether ovulation is happening often enough to allow pregnancy.
If your periods are irregular or unpredictable, trying to stick to traditional methods of ovulation prediction like cycle counting or ovulation test kits may not be helpful. Early assessment with a doctor helps clarify whether continued trying is reasonable or whether support would be more effective.
What a fertility assessment for PCOS usually includes

A fertility assessment aims to identify what is preventing ovulation, fertilisation, or implantation. Implantation is when an embryo attaches to the lining of the uterus. With PCOS, the most common issue is irregular or absent ovulation, but it is not the only factor. A good assessment checks the full picture so you do not treat the wrong problem. This includes reviewing symptoms such as bleeding between periods, which can signal hormonal fluctuations that affect cycle predictability.
Partner assessment matters too. Fertility is shared. Even if PCOS affects ovulation, sperm health and timing can still be limiting factors. Checking both sides early can prevent delays and reduce frustration.
Cycle and symptom history
Doctors usually ask about your cycle pattern and your symptoms. They often ask:
- How long your cycles are, and how much they vary
- When you last had a period
- Whether you notice ovulation signs
- How long have you been trying to conceive
- Past pregnancies, losses, or complications
- Symptoms linked to PCOS, such as acne, excess hair growth, weight changes, or mood changes
- Lifestyle factors, sleep, stress, and exercise patterns
This history matters because it guides what to test and when. It also helps doctors estimate how often you likely ovulate and whether there are red flags that need earlier action.
Blood tests
Blood tests usually check hormones and metabolic health.
Hormone tests can include:
- Luteinising hormone (LH) and follicle-stimulating hormone (FSH)
- Testosterone, sometimes alongside other androgen markers
- Prolactin, which can affect ovulation if it is raised
- Thyroid markers, because thyroid imbalance can disrupt cycles
Metabolic tests can include:
- Glucose tests to check blood sugar regulation
- Lipids, which include cholesterol and triglycerides
These tests help confirm patterns linked to PCOS and identify issues that can affect ovulation and pregnancy health.
Ultrasound

Ultrasound helps assess the follicle pattern and the endometrium. The endometrium is the lining of the uterus. In PCOS, ultrasound may show many small follicles, which fits the common PCOS pattern. Ultrasound can also show endometrial thickness, which can reflect how your cycle hormones are behaving.
Ultrasound can suggest whether ovulation is likely, but it cannot always confirm that ovulation happened unless it is timed and repeated. One scan is a snapshot. It does not replace tracking across time.
Partner assessment and tubal factors
Partner assessment commonly starts with a semen analysis. This test checks sperm count, movement, and shape. It is a practical step because it is non-invasive and can quickly identify whether sperm factors are contributing.
Tubal factors refer to whether the fallopian tubes are open and able to allow sperm and egg to meet. A tubal assessment checks tubal patency, which means openness. This is usually considered when you have been trying for a while, if there are risk factors for tubal blockage, or if ovulation is confirmed but pregnancy is not happening.
Doctor’s Insight: A fertility assessment for PCOS requires a detailed consultation with an experienced doctor to tailor and customize the necessary and suitable tests required for your needs. It is not about running every test available.
Often times, ovulation issues are the most common cause of fertility issues in women with PCOS. When assessment is done early and systematically, it can avoid unnecessary time wasted and allow the couple to get the required help as early as they need.
Fertility treatments pathways for PCOS: what options exist
Fertility treatment for PCOS usually follows a stepwise plan. Doctors start with the least invasive options that can restore ovulation and improve timing. Doctors then progress only if needed. This approach protects your health, reduces unnecessary costs, and avoids overtreatment.
Your plan should also be personalised. Two women can both have PCOS and need very different support. Your cycle pattern, age, metabolic health, and how long you have been trying all shape the best next step.
Lifestyle-first, with clinical targets
Lifestyle changes can improve ovulation for many women, especially when insulin resistance is present. The goal is not rapid weight loss. The goal is better metabolic stability and more predictable hormone signalling.
Where appropriate, doctors may discuss weight and waist circumference targets, as abdominal fat can worsen insulin resistance. Waist circumference can reflect central adiposity, which is fat stored around the abdomen. Even modest, sustained changes can improve ovulation frequency in some women.
Doctors may also track glucose targets. Glucose is blood sugar. If blood sugar runs high, it can worsen insulin resistance and androgen production. Your doctor may use markers such as fasting glucose or HbA1c. HbA1c reflects average blood sugar over about three months. Improving these markers can support cycle regulation and reduce pregnancy risks.
Medical ovulation support
If ovulation remains irregular or absent, doctors may recommend ovulation induction. Ovulation induction means using medicine to help your ovaries mature and release an egg in a more predictable way. The goal is usually one healthy egg release per cycle, not multiple eggs.
Monitoring matters for safety and effectiveness. Doctors may monitor response with ultrasound to check follicle growth and with blood tests when needed. This helps reduce the risk of overstimulation and helps time intercourse or procedures more accurately. Your doctor also considers your overall health, including glucose control, before and during treatment.
When assisted reproduction is considered
Assisted reproduction means helping fertilisation happen outside the body and then placing an embryo into the uterus. This is often called in vitro fertilisation, but you do not need the term to understand the concept. It is a structured option that can bypass some barriers to conception.
Assisted reproduction is not always the first step in PCOS because many women can conceive with earlier interventions, especially if ovulation can be restored. Doctors usually consider assisted reproduction when ovulation support has not worked, when there are additional factors such as tubal blockage or significant sperm issues, or when time is more limited due to age or other clinical reasons.
Pregnancy planning with PCOS: risks you can reduce with preparation
PCOS can increase some pregnancy risks, but preparation can reduce many of them. You do not need to aim for “perfect health” before trying. You need a practical plan that improves metabolic stability, supports early pregnancy, and sets up sensible monitoring. This is especially relevant if you have irregular cycles, insulin resistance, or previous pregnancy complications.
Gestational diabetes and metabolic risk
Gestational diabetes is raised blood sugar that starts during pregnancy. PCOS is associated with a higher risk of insulin resistance, which can further increase this risk. Screening matters because gestational diabetes often has no early symptoms.
Doctors usually screen for gestational diabetes during pregnancy with a glucose test. Some women also benefit from earlier screening if they have risk factors such as prediabetes or a higher body mass index. Prevention focuses on steady blood sugar control through balanced meals, regular movement, and adequate sleep. Doctors may also recommend preconception checks for glucose markers, because improving these before pregnancy can lower risk and simplify pregnancy care.
Blood pressure and pregnancy monitoring
PCOS can be linked with a higher chance of blood pressure issues in pregnancy for some women, especially when metabolic risk is present. Monitoring matters because high blood pressure can affect the placenta and your overall pregnancy health.
Regular blood pressure checks help doctors detect changes early. Early detection supports timely management, which can reduce complications. You also benefit from tracking related factors that influence blood pressure, such as sleep, stress, physical activity, and sodium intake.
Early pregnancy support and follow-up
Early pregnancy support often focuses on confirming location, timing, and viability. If your cycles are irregular, estimating gestational age can be harder, so an early ultrasound can be useful. Doctors usually time an early scan based on your last menstrual period, an ovulation estimate, or a positive pregnancy test, and then use that timing for follow-up. The goal is to confirm that the pregnancy is in the uterus and to check early development at an appropriate time.
You should seek medical advice promptly if you have red flags such as heavy bleeding, severe one-sided pelvic pain, fainting, or worsening dizziness. You should also seek help if you have persistent severe vomiting, fever, or symptoms that feel significantly “off” for you. Early review is protective, not alarmist.
What to expect at your first PCOS fertility consultation
A first consultation should feel structured and practical. You should leave with clarity on whether you are ovulating, what else might be affecting your conception, and what the next steps are. You do not need to arrive with perfect tracking or the “right” answers. You only need enough information for a doctor to build a plan that fits your body and timeline.
What to bring
You can make the visit smoother if you bring:
- Your recent cycle dates, including the first day of each period
- Any ovulation tracking notes, such as ovulation tests or basal body temperature charts
- Previous blood test results and ultrasound reports, if you have them
- A list of medicines and supplements, including doses
- Relevant medical history, including thyroid issues, diabetes risk, or past pregnancy outcomes
- Your partner’s relevant test results, if already done
Questions you can ask
You can use these questions to keep the visit focused.
- Do my cycle pattern and results suggest I am ovulating regularly?
- Which tests do you recommend first, and what will each test clarify?
- Are there signs of insulin resistance or metabolic risk that could affect ovulation?
- What is the most likely reason I am not conceiving yet?
- What should I do for the next one to three cycles while tests are in progress?
- What lifestyle changes will make the biggest difference for my specific pattern?
- When should I consider ovulation induction, and what does monitoring involve?
- What risks should I plan for if I become pregnant, and what screening will I need?
- Should my partner do a semen analysis now, or later?
- What would make you escalate care sooner rather than later?
- What does success look like over the next three months?
- When is the right time for follow-up, and what should I track before then?
What a sensible plan looks like
A sensible plan usually follows a clear sequence. A doctor first confirms whether ovulation is happening and checks for other common fertility factors, such as sperm health and tubal patency. Doctors then match treatment intensity to your findings, age, and how long you have been trying.
You should also expect a follow-up cadence that keeps momentum without creating pressure. Many plans include a review after test results and then review every one to three cycles, depending on what you are doing next. If you start ovulation induction, follow-up is often closer because monitoring is part of safety. The goal is steady progress with clear decision points, not endless waiting.
When to book an appointment if you have PCOS
You should book an appointment when you feel stuck, uncertain, or tired of guessing. Booking is a practical step. It helps you determine whether ovulation is happening and identify what is slowing conception. You also gain a clear plan, which often reduces stress and wasted months. If you are ready to explore PCOS treatment options in Singapore, an assessment can help match you to the right next step.
You do not need to wait until things feel “serious”. You can book proactively to protect your time and give yourself better clarity.
Quick self-check
You should consider booking if any of these apply:
- You have been trying for 12 months without pregnancy, and you are under 35.
- You have been trying for 6 months without pregnancy, and you are 35 or older.
- You have cycles longer than 35 days or cycles that vary widely.
- You miss periods often or go months without bleeding.
- You cannot identify ovulation signs across several cycles.
- You have a known history of insulin resistance, prediabetes, or gestational diabetes.
- You have severe PCOS symptoms that affect daily life.
- You have had a previous pregnancy loss and want a clear plan before trying again.
- You feel anxious, overwhelmed, or exhausted by tracking and uncertainty.
If you tick even one or two of these, an assessment can give you clarity and a realistic next step.
Conclusion
PCOS can make getting pregnant feel uncertain, but many fertility outcomes improve when you focus on the right levers. You improve your chances when you understand whether you are ovulating, time intercourse around a real fertile window, and use targeted help when required. You do not need to manage this alone or keep guessing for months.
You can choose one of three next steps.
- You keep trying naturally, but you track ovulation more consistently, so timing becomes clearer.
- You optimise ovulation support through sustainable nutrition, regular movement, and better sleep and stress control, especially if insulin resistance is likely.
- You book an assessment when your cycles are very irregular, when ovulation is unclear, or when time-based thresholds are met, so you get a plan with clear decision points.
Medical References
- National Institutes of Health (NIH) – MedlinePlus
Polycystic Ovary Syndrome (PCOS): symptoms, hormonal features, and fertility impact.
https://medlineplus.gov/polycysticovarysyndrome.html - National Health Service (NHS), United Kingdom
Fertility in the menstrual cycle and ovulation timing.
https://www.nhs.uk/conditions/periods/fertility-in-the-menstrual-cycle/ - The Endocrine Society
Hormonal mechanisms in PCOS, including LH–FSH imbalance and androgen excess.
https://www.endocrine.org/patient-engagement/endocrine-library/polycystic-ovary-syndrome - American College of Obstetricians and Gynecologists (ACOG)
PCOS overview, fertility implications, and when to seek medical assessment.
https://www.acog.org/womens-health/faqs/polycystic-ovary-syndrome - American Society for Reproductive Medicine (ASRM)
Fertility evaluation, ovulation disorders, and stepwise treatment approaches.
https://www.reproductivefacts.org/ - World Health Organization (WHO)
Infertility definitions and reproductive health principles.
https://www.who.int/health-topics/infertility