Polycystic ovarian syndrome (PCOS) is a common hormonal condition that affects how the ovaries function. It can influence menstrual cycles, hormone levels, and ovulation, which is why symptoms can look very different from one woman to another. Some women notice changes early, while others may not realise something is off until later in life.
This guide explains what PCOS is, how it affects the body, and why symptoms vary so widely. You will learn how PCOS is usually understood and when it may be important to seek medical review. The focus here is upon clarity and understanding, not treatment decisions, so you can recognise what PCOS involves and what it may mean for you.
What Is Polycystic Ovarian Syndrome (PCOS)?
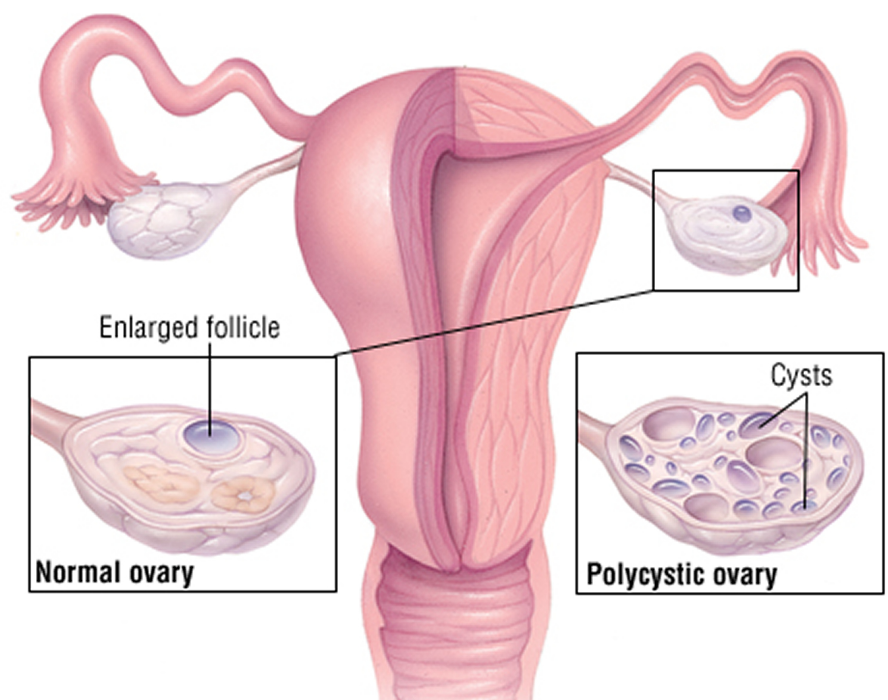
Polycystic ovarian syndrome, often shortened to PCOS, is a hormonal condition that affects how the ovaries function. It mainly involves hormone imbalance and irregular ovulation, which is the process by which an ovary releases an egg each month. PCOS affects an estimated 10–13% of women of reproductive age, based on the International evidence-based PCOS guideline.
Despite its name, PCOS is not defined by ovarian cysts alone. Many women with PCOS do not have cysts on their ovaries, and having cysts is not required for a diagnosis. The name can be misleading, which is why PCOS is better understood by how it affects hormones and ovulation rather than by ultrasound findings alone.
PCOS is called a “syndrome” because it describes a pattern of features rather than a single symptom. These features can appear differently from one person to another. Some women notice menstrual changes early, while others may experience skin concerns, weight changes, or fertility-related issues first. This variability is a key part of understanding PCOS.
How PCOS Affects the Body
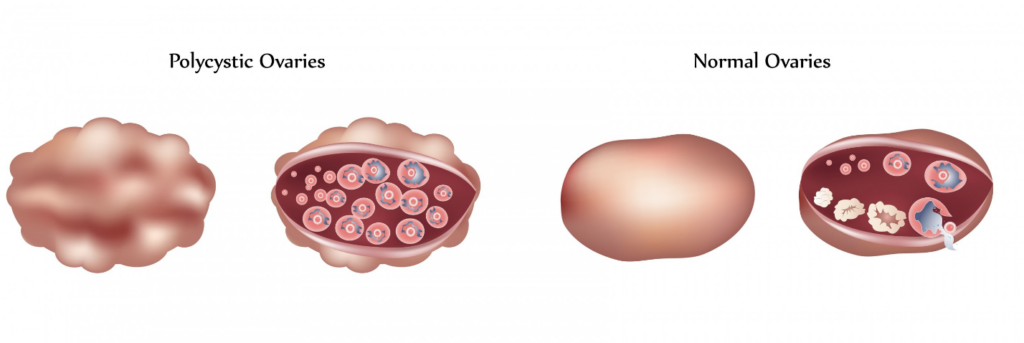
PCOS affects the body through a combination of hormonal changes and disrupted ovulation. Knowing these processes makes it easier to see why symptoms may differ greatly across women.
Hormonal imbalance
Hormones act as chemical messengers that help regulate your menstrual cycle, skin, hair growth, and metabolism. In PCOS, this balance is disrupted. Some hormones may be higher than usual, while others may not follow a regular pattern, which can affect how the ovaries function month to month.
Ovulation disruption
Ovulation is the monthly release of an egg from the ovary. In PCOS, ovulation may happen irregularly or less often. When ovulation is irregular, menstrual cycles can become infrequent, delayed, or unpredictable.
Androgen (male-type hormone) excess
Women naturally produce small amounts of androgens, sometimes referred to as male-type hormones. In PCOS, androgen levels may be higher. This can influence acne, oily skin, excess facial or body hair, and scalp hair thinning.
Insulin resistance, explained simply
Insulin is a hormone that helps your body manage blood sugar. In PCOS, your body may not respond to insulin efficiently. When this happens, insulin levels can rise, which may further disrupt hormone balance and ovulation. Insulin resistance does not always cause obvious symptoms, but it plays an important role in how PCOS affects the body over time.
Common Signs and Symptoms of PCOS
PCOS symptoms often appear as a pattern rather than a single sign. You may have only a few symptoms, and their severity can change over time. This section helps you recognise common patterns, not self-diagnose.
1.Irregular or absent menstrual cycles

Irregular periods are one of the most common features of PCOS. You may notice long gaps between periods, unpredictable timing, or periods that stop for months at a time. These changes often reflect irregular ovulation and are further explained in our guide on irregular periods.
2. Acne and increased facial or body hair

Higher androgen levels can contribute to persistent acne, oily skin, and increased facial or body hair growth. Some women also notice scalp hair thinning. These changes can develop gradually and may persist beyond the teenage years. If acne is a key concern, you can learn more about PCOS and hormonal acne.
3. Fertility challenges related to ovulation

PCOS can affect how regularly ovulation occurs. When ovulation is infrequent or unpredictable, it can be harder to identify fertile windows and time attempts to conceive. This does not mean pregnancy is impossible, but it can make planning more difficult for some women.
4. Weight and metabolic changes

Some women with PCOS gain weight more easily, particularly around the abdomen, while others do not. PCOS can occur at any body size. Metabolic changes are often linked to insulin resistance, which affects how the body manages blood sugar and may contribute to fatigue or energy fluctuations.
5. Mood and emotional changes
Living with ongoing symptoms can affect emotional well-being. Low mood, anxiety, frustration, and body image concerns are not uncommon, especially when symptoms involve skin, hair, weight, or fertility worries.
6. Endometrial health concerns
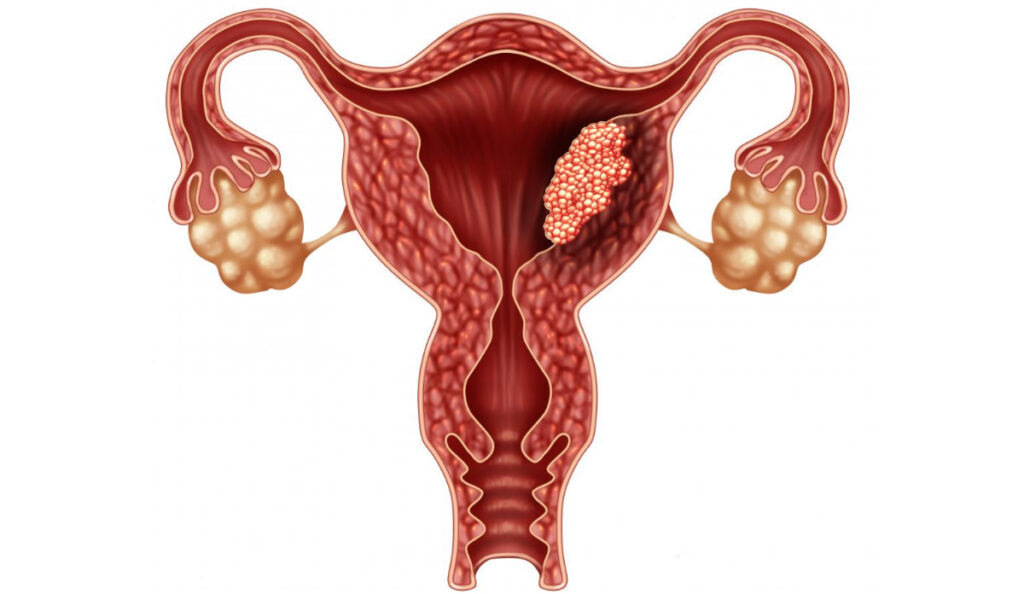
When menstrual cycles are very infrequent, the lining can remain thicker between cycles. This is why persistent long gaps between periods should be discussed with a clinician. This is a monitoring issue for most women, and it is best assessed in the context of your cycle pattern and overall health, including whether cycle regulation may be appropriate, such as birth control for PCOS.
What Causes PCOS
PCOS does not have a single cause, and it is not something you caused through lifestyle choices. It develops from a combination of biological factors that affect how hormones and ovulation are regulated.
Genetic factors
PCOS often runs in families. If close relatives have PCOS, irregular periods, or type 2 diabetes, your likelihood of developing PCOS may be higher. Genetics influences risk, but it does not determine how severe symptoms will be.
Hormonal regulation issues
PCOS involves disrupted hormone signalling between the brain and the ovaries. This can lead to higher androgen levels and irregular ovulation, which then affects menstrual cycles, skin, hair, and fertility patterns.
Insulin resistance as a driver
For many women, insulin resistance plays a central role. Insulin is a hormone that helps manage blood sugar. When the body does not respond to insulin efficiently, insulin levels can rise and stimulate the ovaries to produce more androgens. This can worsen cycle irregularity and other symptoms. Importantly, insulin resistance can be present regardless of body size.
How PCOS Is Diagnosed
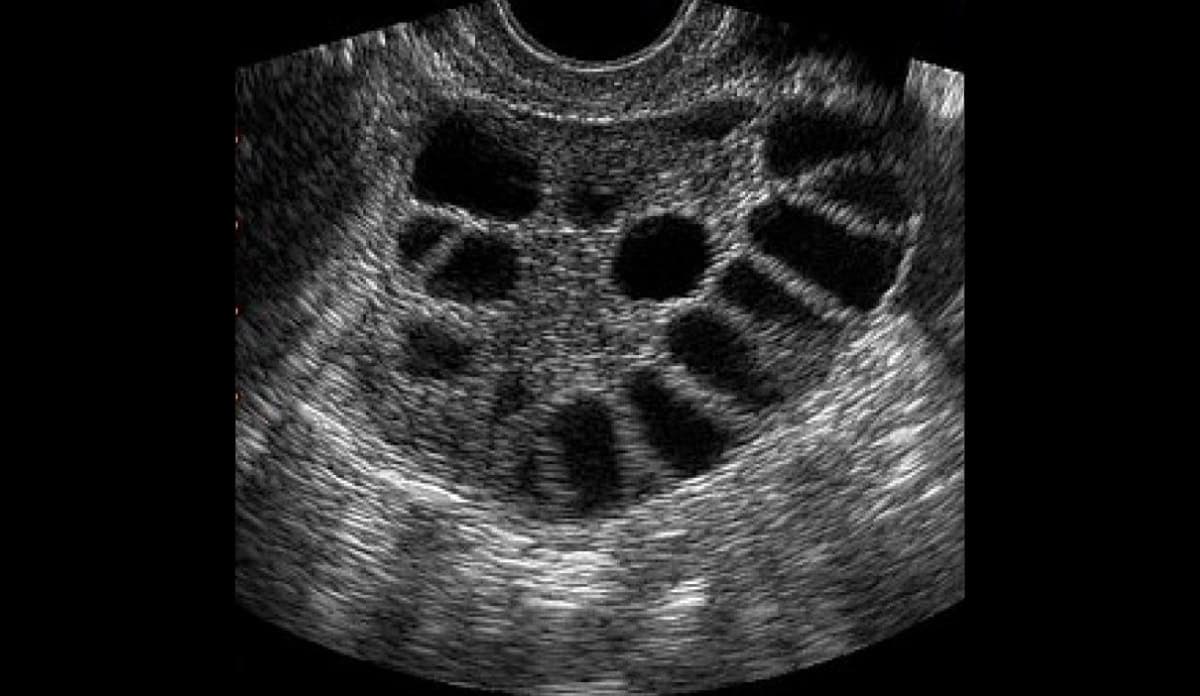
Many women are assessed for PCOS after noticing irregular periods or signs linked to higher androgen levels (for example, acne or excess facial or body hair). Doctors diagnose PCOS by looking at a pattern of features rather than relying on one single test.
PCOS is commonly diagnosed using the Rotterdam criteria. This approach supports a PCOS diagnosis when two out of three features are present:
- Irregular or infrequent ovulation, often shown by irregular periods
- Clinical or biochemical signs of higher androgen levels (such as acne, excess hair growth, or blood test findings)
- An ultrasound pattern that may show polycystic ovarian morphology
Your doctor may use hormone blood tests and a pelvic ultrasound to support the assessment. Additional tests may also be done to check metabolic health, such as blood sugar, because PCOS can be associated with insulin resistance.
Not everyone will have abnormal blood tests or a polycystic appearance on ultrasound. Diagnosis is based on the overall picture, which is why the process is individualised.
Doctor’s Insight:
As a doctor who has treated many women with Polycystic Ovary Syndrome (PCOS) over the years, it is important to recognise that PCOS can present very differently from person to person. Some women with PCOS are overweight, while others may be a healthy weight or physically active.
Proper diagnosis typically requires a combination of hormonal blood tests and an ultrasound scan. Findings may appear in one test but not the other, so both help provide a clearer overall picture.
PCOS involves a cluster of symptoms that can affect multiple aspects of your health. Regular screening supports early detection and helps reduce the risk of longer-term complications.
PCOS Across Different Life Stages
PCOS can look different at various stages of life. Symptoms may change over time, which is why PCOS is often recognised and managed differently depending on age and life circumstances.
PCOS in teenagers
In adolescence, PCOS may first appear as irregular periods, persistent acne, or excess hair growth. Because menstrual cycles can be naturally irregular in the early years after puberty, PCOS may not be diagnosed immediately. Ongoing symptoms that persist beyond this adjustment phase are more likely to prompt further assessment.
PCOS during reproductive years
During the reproductive years, PCOS is often identified due to menstrual irregularity, skin or hair concerns, or difficulty conceiving. Some women may notice changes after weight fluctuations, stress, or lifestyle changes, while others have stable symptoms over many years. Fertility planning often brings PCOS into focus at this stage.
PCOS approaching perimenopause
As women approach perimenopause, menstrual cycles naturally become less regular, which can make PCOS harder to distinguish. Hormonal patterns change, but metabolic risks associated with PCOS, such as insulin resistance, may persist. Monitoring overall health remains important even as reproductive symptoms evolve.
Endometrial Health and PCOS
PCOS can affect the lining of the uterus, known as the endometrium, particularly when menstrual cycles are very irregular or occur infrequently. Understanding this helps explain why cycle patterns matter, even if periods are not causing discomfort.
Why irregular cycles affect the uterine lining
During a regular menstrual cycle, hormones help the uterine lining build up and shed in a predictable way. When ovulation does not occur regularly, the lining may continue to thicken without being shed. Over time, this can lead to changes that need medical attention.
What endometrial hyperplasia means
Endometrial hyperplasia refers to a thickening of the uterine lining. It is not cancer, but it can increase risk if left unmonitored for long periods. This condition is more likely when there are prolonged gaps between periods, which is why ongoing cycle irregularity should be assessed rather than ignored.
Why monitoring matters
For most women with PCOS, endometrial health is a monitoring issue rather than an immediate concern. Regular review helps ensure the uterine lining remains healthy and allows changes to be addressed early if needed. Monitoring is part of good long-term care and supports overall reproductive health.
Common PCOS Myths and Misunderstandings
PCOS is often misunderstood, which can lead to unnecessary worry or delayed care. Clearing up common myths helps you understand what PCOS is — and what it is not.
You must have cysts to have PCOS
This is one of the most common misconceptions. You do not need to have ovarian cysts to have PCOS. Many women with PCOS have normal-looking ovaries on ultrasound. PCOS is defined by hormone patterns and ovulation changes, not cysts alone.
PCOS is caused by weight
PCOS is not caused by weight. While weight changes can influence symptoms for some women, PCOS occurs in women of all body sizes. Hormone regulation, genetics, and insulin resistance play a much larger role than weight alone.
Pregnancy is impossible with PCOS
PCOS does not mean you cannot get pregnant. Many women with PCOS conceive, either naturally or with medical support. Fertility may be less predictable for some women due to irregular ovulation, but pregnancy is very much possible.
When PCOS Needs Medical Attention
PCOS does not always require immediate treatment, but there are situations where medical review matters. The aim is not to intervene early for everyone, but to recognise when monitoring or support is important.
You should consider seeing a doctor if you have persistent or worsening symptoms. This includes irregular periods that continue over time, acne or excess hair growth that does not improve, or symptoms that begin to interfere with your quality of life.
Ongoing irregular periods deserve medical review, especially when there are long gaps between cycles. Infrequent periods can affect endometrial health over time, which is why cycle patterns should not be ignored even if they are not painful or disruptive.
You should also seek advice if you have fertility planning concerns. If you are trying to conceive, or planning to do so in the near future, an assessment can help clarify ovulation patterns and guide next steps without unnecessary delay.
Metabolic health concerns are another reason to get checked. Changes in weight, rising blood sugar, high blood pressure, or cholesterol issues may not cause obvious symptoms at first, but they are important to address early in women with PCOS.
If you want to understand what assessment and care can involve, you can read more about polycystic ovarian syndrome.
PCOS is a common condition, but it does not affect everyone in the same way. Symptoms can change over time, and their impact varies between individuals. Understanding what PCOS is and how it affects the body helps you recognise patterns, separate myths from facts, and know when medical review may be helpful. With proper assessment and ongoing awareness, PCOS can be managed thoughtfully at different stages of life, supporting both short-term wellbeing and long-term health.
Medical References:
- International evidence-based guideline for the assessment and management of polycystic ovary syndrome (PCOS), led by Monash University and global endocrine and reproductive health organisations
- Royal College of Obstetricians and Gynaecologists (RCOG) – Polycystic Ovary Syndrome (PCOS) patient information
- NHS UK – Polycystic ovary syndrome (PCOS)
- Endocrine Society – Polycystic Ovary Syndrome